It goes without saying that since the beginning of this pandemic, healthcare professionals’ commitment to fighting the virus and keeping their communities safe has been incredible.
Those individuals with the most first-hand experience of the severity of symptoms and spread have been tirelessly working in stretched conditions over the past few months but their own wellbeing and mental health should not be forgotten. Not only are they working overtime and in high pressure, flawed circumstances, it has been reported in Italy that health workers make up around 9% of the nation’s cases.
Whilst up against the unprecedented condition, with strained resources, treating the crisis on the frontline is forcing HCPs to balance self-care and protecting their families and their vow to treat patients. Support from employers and other health stakeholders is crucial for the sustained welfare of medical staff during, and beyond, this pandemic.
Within the tens of millions of posts on COVID-19 each day, no strangers to Twitter, HCPs are contributing to the online conversation and facilitating the global reach of correct information. Beyond medical information sharing, HCPs have been sharing their unique perspectives on the pandemic, offering insight into their victories, fears, personal breakthroughs and anxieties.
Throughout March and April, CREATION Pinpoint identified HCP conversations discussing wellbeing in the context of COVID-19 across the globe, including in North and South America, Europe and Asia. The content of these posts can range from conversations about symptoms including stress, anxiety, burnout, emotional burden and psychological trauma as well as to mental health support from peers, employers and other organisations.
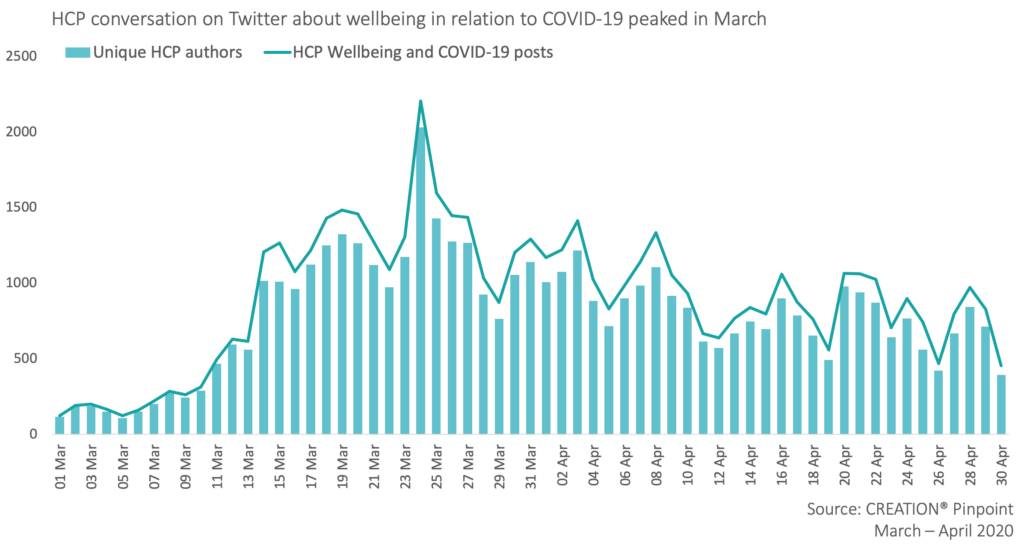
HCPs are discussing their COVID-19 concerns online
Each day when an HCP arrives at a hospital or clinic treating COVID-19 patients they are forced to contradict government guidance for the rest of the population on social distancing, in order to maintain quality patient care. HCPs globally are highlighting the stress and fear associated with this, and applauding their colleagues who continue to do their jobs in such circumstances.
Working 12 of the last 14 days, I am amazed at how my colleagues, the staff, and the residents have faced the rising COVID stress to continue providing amazing patient care. #Cincyproud #together @CincyPHMFellows @CincyMedPeds @CincyChildrens @CincyPedsRes @CincyPHM pic.twitter.com/7zg6TiOA8e
— Ben Kinnear (@Midwest_MedPeds) March 22, 2020
Published in Nursing Standard, HCPs shared the perspective of an Italian nurse who posted an image of her face covered in bruises from her personal protective equipment (PPE), which displayed both a physical and psychological exhaustion, as well as the place of fear of contracting the virus.
A nurse caring for patients with #Covid_19 in Italy has shared a picture of her face bruised from wearing a protective mask.
Alessia Bonari said she was ‘physically and psychologically’ tired from caring for patients during the pandemic.https://t.co/GQv45UHnkf— Nursing Standard (@NurseStandard) March 13, 2020
HCPs without proper PPE have been sharing their circumstances and searching for better provisions. One NHS worker commented on NHS chief Sir Simon Stevens’ statement claiming that all NHS staff have required PPE, saying that this was not the case, causing such staff to feel unsafe.
Listening to the chief of the NHS ( sir Simon Stevens) talking on live tv about #coronavirus . He says all #NHS staff should and do have access to the required PPE. Er, afraid not ! I know for a fact nhs staff are seeing patients UNPROTECTED. This isn’t safe. We don’t feel safe !
— Ben (@BendyBen999) March 17, 2020
Understanding the HCP perspective, as shared on Twitter, can allow the NHS and NGOs supplying these provisions to align with HCPs’ daily experience. Frontline workers have spoken of the fear and anxiety they are feeling due to a lack of PPE. Some have been able to turn to telemedicine, such as this cardiac electrophysiologist in the US:
I am STAYING HOME and seeing patients through video conferencing everyday so they don't have to go to the hospital & contract COVID19.
I am fearing lack of #PPE for urgent medical procedures I might have to do.
I am talking to policy makers & expressing my concerns. https://t.co/j3dIaeGoX5
— Kashif Chaudhry (@KashifMD) March 25, 2020
A further cause for concern among HCPs when treating patients is their own lack of testing. A neurology resident, Lucia Li, working in London, summarised her opinion after another neurosurgeon wrote about his experience treating a positive COVID-19 patient without PPE, or testing. Both individuals called on Matt Hancock to explain this situation.
Lack of testing for #NHS staff v puzzling – if neg, can work without worry; if pos, can quarantine immediately. Not knowing is stressful for us, and dangerous for our patients @MattHancock – pls sort this out. https://t.co/mvan4Pj4hD
— Lucia Li (@NeuroDocLucia) March 17, 2020
Hundreds of doctors tweeted about access to testing for medical staff and how the results allows them to more safely and comfortably do their jobs. Highlighting the need for more clarity, many others asked questions to health and government leaders: Matt Hancock, Dr Nikita Kanani, Boris Johnson and Donald Trump.
The *single* biggest anxiety for us all at work currently; the complete lack of PPE. And the torrent of patients has yet to even start..https://t.co/DmZPqaiIBF
— Paul Lancaster (@lancs7) March 17, 2020
HCPs have posted about the choice between serving patients and protecting their families by self-isolating at home. Not only are they facing protective measures in the workplace, but they are having to sacrifice time with their family for fear of them becoming infected.
Unable to sleep (again!) due to #COVID19 stress.
Never suffered Insomnia before!
Feel scared for my family & team.
Mental health impact on doctors & frontline #NHS staff is very real.
Hope people feel more able to share.
We need kindness & protection too! @TheBMA #OurNHSPeople— Gaurav Gupta (@drguptagaurav) April 12, 2020
HCPs have sought support from their hospitals to allow them to continue working safely without putting their families at risk. Jennifer Weiss, a pediatric orthopedist in the US, asked her peers for their experiences using the Twitter hashtag #MedTwitter.
#Medtwitter has anyone’s hospital created a space for doctors and clinicians to stay away from their families if there is fear of exposure to #COVID19? We are all committed to taking care of patients and also trying to keep our families safe.
— Jennifer Weiss (@mymomthesurgeon) March 17, 2020
Mental health support is essential for HCPs
Not only are HCPs seeking provision for PPE, testing and accommodation, but there is an increasing conversation about mental health support, specifically for these clinical staff. Citing COVID-related mental health data, Candian Internist Lisa Richardson said it was critical for such support to be in place.
In a study of 1300 healthcare workers exposed to #COVID19, 50% had symptoms of depression, 45% anxiety, 34% insomnia & 72% distress. Nurses, women & frontline workers had more severe symptoms.
Self-care & mental health support are critical right now.https://t.co/40ePTOZhwl
— Lisa Richardson MD (@RicharLisa) March 24, 2020
Elsewhere, frontline staff, such as an NHS nurse, used Twitter to ask whether there was any mental health support available, again tagging policy and government leaders for a response. HCPs using social media to reach out to those in leadership positions, able to induce change, is a common behaviour during this time when they are desperate for such change and answers to questions that hundreds of health staff are asking.
I would like to thank EVERY SINGLE ONE OF my patients for…asking me how I am on my visits & actually wanting an answer.
Not the psychiatrist answer ("good" or "what makes u ask?")
The REAL one.
It means a lot to me that u care about me as a human.#Covid_19 #mentalhealth pic.twitter.com/3uF4nHeSKo
— Jessi Gold MD MS (@drjessigold) April 24, 2020
Thank you @DShepYEG for meeting with us last night, for really listening to our concerns & validating our stress & feelings as Alberta family docs during this unprecedented #covid19 #pandemic. That this is in the context of lack of gov't support is demoralizing. #ABdocs4patients https://t.co/Hu9yUg6F6y
— Dr. Amy Tan (@AmyTanMD) March 14, 2020
As expressed by psychiatrist Dr Jessi Gold and family physician Dr Amy Tan, HCPs are human and their needs should be listened to.
Listen now for a brighter future
When an unmet need is discovered, those in a position to provide help, including in healthcare and government, should unite together in support. Listening now and acting on the conversation HCPs are having among themselves online will not only be of benefit to HCPs in the short term, but will allow for post-COVID preparation for essential ongoing support and engagement.
Health stakeholders have an opportunity to improve systems and increase sustainability of communication following this pandemic, to work together for a brighter future.
CREATION.co has been tracking the online HCP conversation relating to coronavirus since the start of the outbreak and is committed to supporting healthcare stakeholders globally. For more insights for strategy and engagement during the COVID-19 pandemic, visit creation.co/knowledge/category/covid19/.
 By Mary Kangley
By Mary Kangley