We have known for a while now that factors such as a rapidly ageing population and rapidly changing patient expectations are contributing to gaps in NHS funding. The intersection of advances in technology, the need to be financially efficient, and the need for positive health outcomes to be put forward has significantly altered both treatment and decision-making processes within the NHS. A new study, conducted by Creation Healthcare, focuses on one particular type of healthcare professionals to analyse what topics and aspects of the healthcare system really matter to pharmacists in the UK– a group whose conversations may hold the key to implementing changes that benefit patients and physicians, as well as delivering the best possible health outcomes.
Pharmacists make their voices heard
Recognising that focusing solely on prescribing data does not give an accurate picture of whether medication-based treatment is as cost-effective and evidence-based as it should be, the Royal Pharmaceutical Society initiated a series of programmes aimed at optimising patient experience and medicine use by reducing wastage, improving adherence and efficacy rates, and eliminating unnecessary medicine consumption.
Health Education England is currently also in the process of implementing pharmacy education and training reforms aimed at measuring and improving pharmacists’ consultation and public health skills in order to support the national health agenda.
In the meantime, numerous UK-based pharmacists and pharmacology experts are making their voices heard via public social media, tweeting about pharmacy-related modules, writing about transforming urgent care services, or blogging about the relationship between community pharmacies and GP surgeries.
Community Pharmacy Services: Acting as the first port-of-call
The data in the study shows that the most discussed topic among healthcare professionals interested in pharmacy is the role of community or local pharmacies, followed by practical discussions around prescription technicalities, such as pressure to grow prescription volumes, re-classification of medicines, and picking up contraindications.
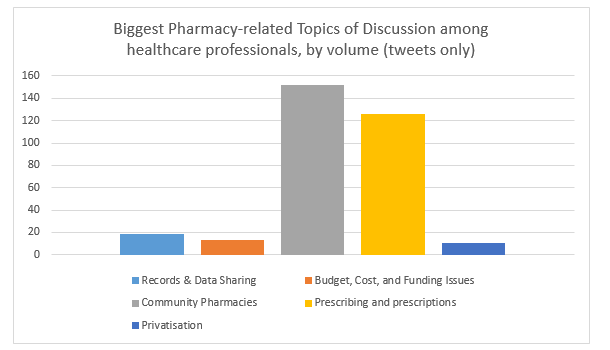
Data from Creation Pinpoint shows that the biggest topics among healthcare professionals talking about pharmacy were the role of community pharmacies, followed by prescribing-related topics.
The most shared tweet in the community pharmacy category is a link to a picture of a Hepatitis C testing kit, indicating the implementation of the service in a Plymouth community pharmacy. The tweet sent by community pharmacist Tom Kallis stirs discussions about the piloting of the project, with other healthcare professionals occasionally weighing in and asking about how the programme is going.
Getting ready to bring rapid hep c testing into our community pharmacy! pic.twitter.com/8zgEV62FUn
— Tom Kallis (@TK_MPharm) January 8, 2015
Pharmacist Tom Kallis’ tweet prompted 14 re-tweets. With infectious disease being such a current topic in the universe of healthcare, healthcare professionals are hopeful that bringing screening to community pharmacies may assist with prevention.
Pharmacists also use microblogging to find dependable statistics and resources that can support their work. Mohammed Hussain, a Leeds-based pharmacist and a member of the General Pharmaceutical Council, turned to Twitter to find out what percentage of health-related community pharmacy consultations happen out-of-hours: “Help please: Anybody know the % of health related community pharmacy consultations that occur OOHs per year/month or week? @rpharms”, he tweeted. Although the question was re-tweeted by 2 healthcare professionals, there was no visible reply on the website. It is possible to interpret this as potential indication of a lack of accessible, digital resources for pharmacy specialists. The wealth of data on prescription-related concerns uncovers a complex framework of issues that tie into multiple aspects of the healthcare-professional-to-patient dynamic, including access to patient notes and data sharing. When a former psychiatric nurse and head of the Drug Information Agency posted a link to a patient in Dumfries who was prescribed potentially toxic medicine, another Scotland-based pharmacist responded by highlighting how difficult it is for such errors to be revealed in good time, but adding that in-pharmacy review can be helpful in such situations: “Dumfries Surgery prescribed ‘toxic’ medicine to patient-Could a Pharmacist have prevented or alerted this happening?…”, tweeted David Grieve, former psychiatric nurse and head of the Drug Information Agency, based in Dumfries. “@davidlgrieve the answer to this is ‘maybe’”, responded Jonathan Burton, a pharmacist based in Scotland. “Very difficult without access to pt notes, but pt counselling/review often uncovers errors.”
Asthma and Urgent Care Most Discussed Services
In terms of management and treatment of long-term conditions, the topic of emergency medicine and urgent care has been the most pressing, with a variety of programmes and pilots across the country that seek to discover whether it is feasible for pharmacists to offer such services. This perhaps reflects views among healthcare professionals about weaknesses in the current healthcare system, revealing the need to delegate emergency medicine related tasks to healthcare professionals outside of surgeries and practices. 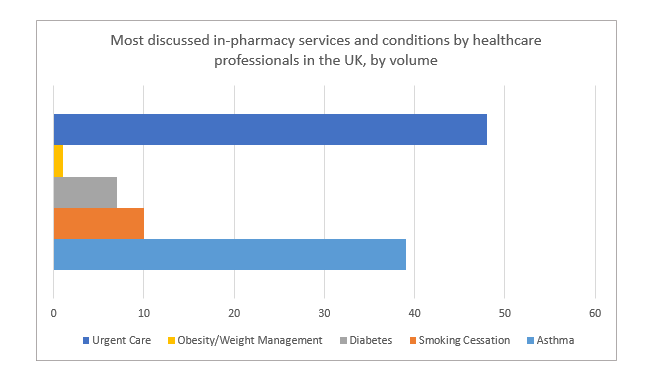 Data taken from Creation Pinpoint shows the most frequently discussed in-pharmacy services in the UK (January-March 2015).
Data taken from Creation Pinpoint shows the most frequently discussed in-pharmacy services in the UK (January-March 2015).
Dr. Judith Smith, Non-Executive Director at the Birmingham Children’s Hospital NHS Foundation Trust, linked to a blog post by a fellow healthcare professional. In the entry, complete with a video interview, Professor Keith Willett, Director of Acute Episodes of Care at NHS England, states that there is real potential for pharmacies to make a difference in this respect.
Is pharmacy part of the solution to emergency care pressures? Keith Willett of @NHSEngland sets out his thoughts: http://t.co/9wQCS740GM — Judith Smith (@DrJudithSmith) January 10, 2015
Dr Judith Smith’s (Director of Policy at @NuffieldTrust and Non-Executive Director at the Birmingham Children’s Hospital NHS Foundation Trust) tweet prompted 6 re-tweets and 6 favourites.
Professor Keith Willett states that pharmacists are one of the most ‘under-appreciated groups’ in healthcare and often have a lot of impact on care without even realising it.
With regards to the relatively high volume of asthma-related tweets, healthcare professionals seem to have picked up on a number of digital initiatives coming from @AsthmaUK, including an informative leaflet tweeted by the organisation, which was re-tweeted 39 times.
Got questions about your asthma or medicines? Your local pharmacist can help: pic.twitter.com/a3REV67ARy
— Asthma UK (@asthmauk) January 26, 2015
Asthma UK’s tweet gains traction by attaching a shareable graphic explaining when it is appropriate to see one’s local pharmacist about various symptoms.
Healthcare professionals and pharmacists also discussed the process of giving asthma patients advice on correct use of inhalers.
There are numerous other issues that UK-based pharmacists face, such as actions taken as a response to honest dispensing errors and galvanising staff in order to advance efforts towards innovation. There is a dynamic set of digitally active pharmacists who, using public social media to communicate with healthcare professionals around the UK, regularly strive to communicate with their peers. Pharmacists constitute an essential group of healthcare professionals and may hold the key to driving real NHS reform, as well as making care more efficient and improving public health outcomes.

