Online healthcare professionals (eHCPs) are interested in treatment options for ulcerative colitis and have shown excitement about emerging options. But we asked ourselves, what else do they discuss?
Using CREATION Pinpoint, we analysed 14,612 unprompted posts about ulcerative colitis written by eHCPs around the world. Imagine these eHCPs are in their hospital break room together and they start discussing their work life in ulcerative colitis, what organically comes up?
While there are some conversations about pharmaceutical treatments (583 mentions, 4% of posts) much of that is driven by responding to news (79% of treatment posts were shares / retweets).
Companies in the UC space providing treatments should be providing good data, good guidance and answering product-related questions. However, they should also show they care about the above-brand needs of their HCPs and, importantly, their patients.
Ulcerative colitis, as such a life-altering disease, is a space where eHCPs care deeply for their patients and their daily life struggles. Three other themes emerged from eHCP which will explore: research in the area of diet and food, insurance denials and medical education.
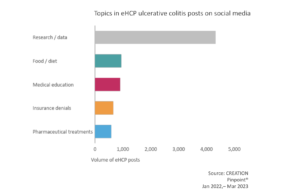
HCPs share the latest research around diet
eHCPs love to share data with their peers on social media (30% of posts related to research, studies or data), the data discussed is not only drug-related data, or even treatment-related data in general. The conversation also covers research into risks of comorbidities and improving the diagnosis process (among other topics).
Within this active conversation about trials we saw eHCPs sharing results and their thoughts on how refined or ultra-processed foods have contributed to the global burden of chronic inflammatory diseases such as inflammatory bowel disease in part via detrimental effects on the gut microbiota (143 eHCP mentions).
Ultraprocessed foods have contributed to the global burden of chronic inflammatory diseases such as inflammatory bowel disease in part via detrimental effects on the gut microbiota. ????????????#MedTwitter #diet #nutrition #IBD #microbiome #health https://t.co/AWumd34SMa pic.twitter.com/RieuXmBgAO
— John Damianos, M.D. (@john_damianosMD) August 9, 2022
As eHCPs discuss gut microbiota and changes in the microbiome, it becomes clear there is a belief this may be a key contributing factor in the rise in IBD prevalence. eHCPs widely shared clinical nutrition guidelines for those working in IBD (27 eHCP shares), which included guidance on microbiota modulation.
Burden on patients of insurance denials
Many posts, especially from eHCPs in the US, expressed concern about patients being denied insurance for their ulcerative colitis treatments. Sharing these stories, HCPs vented their frustrations and made it clear they want better and easier access to medications for their patients.
One particular story published on ProPublica sparked a lot of online conversation. Enraged eHCPs gave evidence for care being denied to a patient, and lamented the lack of empathy shown to patients.
“A doctor paid by United concluded that denying payments for McNaughton’s treatment could put his health at risk, but the company buried his report.”
On recorded line, @UHC employees laugh about denying care.https://t.co/8q5MocalQJ
— Rich Duszak, MD (@RichDuszak) March 6, 2023
Medical education
HCPs are using social media as a space to amplify opportunities for furthering medical education in ulcerative colitis. They often use the hashtag #MedEd.
Webinars hosted by the United European Gastroenterology (UEG) were designed as a place to “learn and discuss with experts in real-time”. Links to these webinars were seen in 70 eHCP posts. Posts published by a non-profit ‘IBD Horizons’ were shared more than 100 times by eHCPs as they work with a team of experts to provide free education.
????@MaiaKayalMD leads Pacific Northwest #IBDHorizons23 6th session in Seattle!!
????Managing Complex #IBD as 2nd Opinion
????A little about Dr Kayal????FREE registration: https://t.co/dRnaco6FEc#MedEd #Crohns #UlcerativeColitis #Gastroenterology #GITwitter pic.twitter.com/MkosoKwCja
— IBD Horizons (@IBDHorizons) March 6, 2023
Another way eHCPs educate their peers is through their conference #IBDHorizons23 (67 eHCP mentions) which was copublished on Instagram, by Dr Anita Afzali (ibd_afzali)
View this post on Instagram
Meet eHCPs unmet needs
Advice for a company working with HCPs in support of ulcerative colitis patients would be to continue to keep them up to speed on clinical and real world data relating to current and emerging therapies but also engage on the other issues that eHCPs are interested in. Analysis of the unprompted online conversation can reveal these issues without introducing survey bias.
In ulcerative colitis eHCPs care deeply about the burden for patients of managing their diet, and managing the cost of treating the disease.
They use digital channels to collaborate with non-profit organisations including United European Gastroenterology and IBD Horizons, and to share learning opportunities with one another
 By Jamie Doggett
By Jamie Doggett